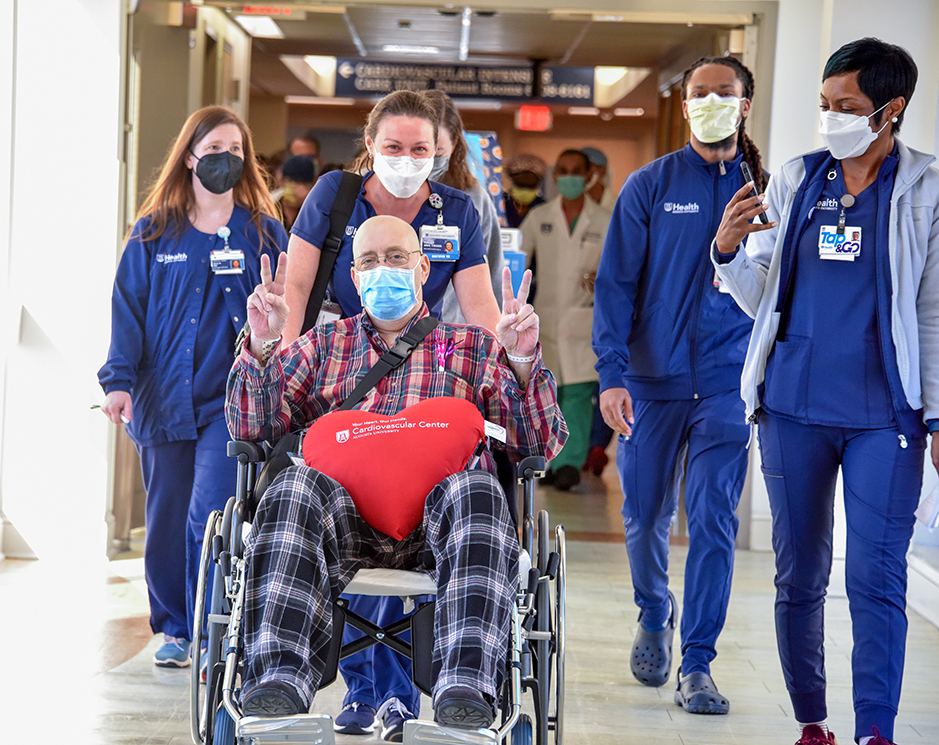
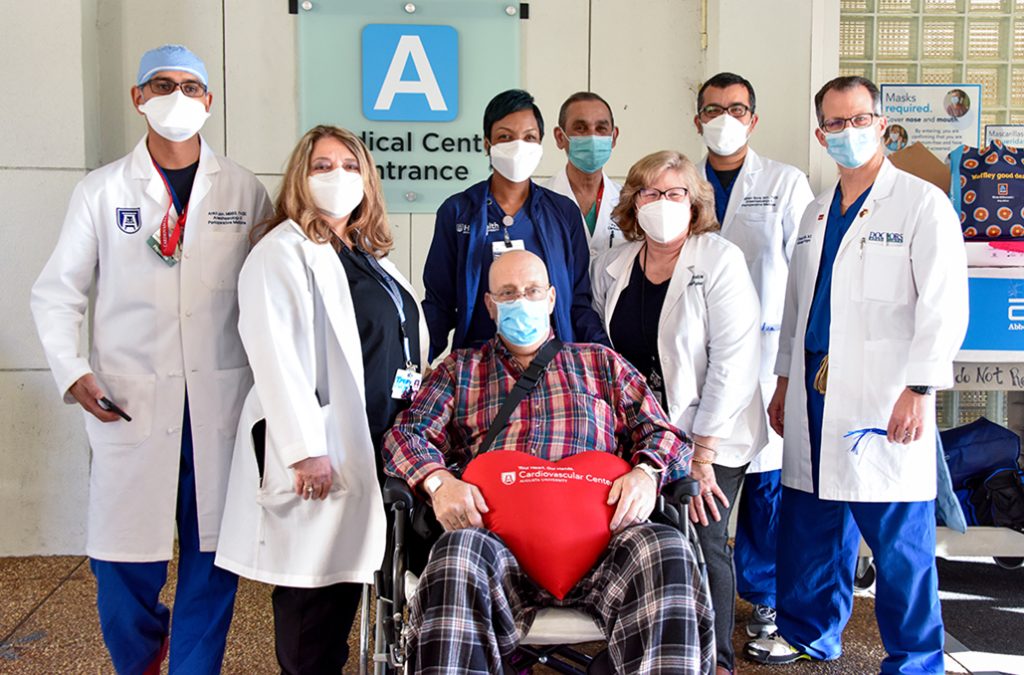
Carefully, Erik Schreiber rose out of his wheelchair and began walking toward the exit of the new Cardiovascular Intensive Care Unit at AU Health, fist-bumping health care workers who lined the halls celebrating his discharge.
The 58-year-old has been living with heart failure for nearly a decade, which recently became severe.
Last month, he received a Left Ventricular Assist Device (LVAD), the first ever implanted at AU Health. The device is implanted into his heart and will improve his heart function, which will allow him to get back to doing the things he loves – and will likely extend his life.
More than 6.2 million adults in the United States are living with heart failure. It is the leading cause of death in the United States.
A failing heart severely limits a patient’s quality of life. They’ll have trouble breathing, gain water weight but lose muscle, and feel extremely tired and weak. It also has a drastic effect on the family around them, as prognosis is bleak.
“The purpose of the device is to improve patients’ quality of life and extend it. In most of these cases, they don’t have many years to live, so this is their opportunity to live longer, and improve their quality of life,” said LVAD coordinator Kianna Curtis. “Like the patient we have right now, his goal was just that he wanted to mow his lawn again.”
LVAD significantly increases the amount of blood flow and reduces the risk of blood clots within the device, or stroke.
The device is implanted into the left ventricle of the heart and powered by an external power supply –either a battery pack or power cord – through a driveline that exits the body.
“It’s replacing the work of the left heart, which has been failing for some time,” said cardiac surgeon Dr. Vijay Patel, who came to AU Health to build the program.
LVAD Medical Director Dr. Stephanie Dunlap, who also came to AU Health to start the assist device program, said instead of being admitted to the hospital every few weeks for heart failure exacerbations, patients would now be able to go months or even years before their next hospital admission.
For some patients, the device can be used to improve quality of life until they can receive a heart transplant. But for most patients for whom transplant isn’t an option, LVAD can help them get back to doing the things they love.
“The big picture is this is a chronic disease. It’s progressive. It carries a very high mortality rate that is higher than most cancers. As they get sicker, their symptoms – and the overall burden – takes a toll on them and their loved ones,” said cardiologist Dr. Evan Hiner. “We have the service now to help them improve their quality of life, which is the LVAD.”
The first patient to receive the implant, for whom Dunlap cared for a year and a half, is currently doing well. Before getting the implant, he suffered severe heart failure for months and an “almost lethal arrhythmia caused him to come to the hospital to be admitted,” Patel said.
Over the next two or three weeks, doctors worked to get his heart failure and irregular heartbeats under control before they could implant the device. Fortunately, he was able to receive the device Jan. 11 as scheduled, Patel said. He was extubated three days later and by the end of Week 1, he was walking around the unit and his wounds were healing well.
Patients will work with a coordinator prior to consenting to an implant, as there is an intense educational period that goes over not only how the device works, but how life will change after surgery. For instance, a wound where the driveline exits the body will have to have sterile dressing changes every day, and the device will need to be connected to power at all times.
“They’re not going to be able to go swimming or take baths, or get on a boat in the middle of the lake,” Curtis said. “That another lifestyle change for these patients.”
But for patients who want just a little more time to see a daughter get married, meet a new grandchild or go back to mowing their lawn, for example, the LVAD can help make it a reality.
Patients who would like more information can call 706-755-8106 to be connected to a member of the LVAD team.